- Forty-five percent of all deaths in children under 5 are attributable to undernutrition
- One hundred forty eight million children suffer from stunting — low height due to malnutrition
- Forty five million children suffer from wasting — low weight due to malnutrition
- The first 1,000 days of a child's life are critical to addressing malnutrition
The story of Community Management of Acute Malnutrition (CMAM) is quintessentially Concern: a listen-first approach developed in partnership with communities that balances innovation with simplicity. A whole greater than the sum of its parts.
The Challenge
For years, centralized in-patient treatment centers were the accepted approach for treating acute malnutrition in children under 5. Logical in theory, it was failing in practice. The cost of running these centers was high, as they required 24/7 staffing. Oftentimes the effort to reach these centers was too much for families seeking care. Mothers would often have to journey —by foot — for days to reach a treatment center. This meant leaving their work and other children behind. As one mother in Ethiopia, Hekuat Kahsay Fanta, told us: “If I leave my other children at home, I close the door on them. To save one life, I can lose the rest of my children.”
Concern’s former International Program Director Anne O’Mahony explains further: “More and more, it became clear that center-based care wasn’t the solution.”
“If I leave my other children at home, I close the door on them. To save one life, I can lose the rest of my children.”
A World-Changing Partnership
In the 1990s Concern partnered with Dr. Steve Collins and his humanitarian research organization Valid to find a solution. We found that the limiting factor to treating malnutrition wasn’t the medical care itself, but how to access it: we needed to de-centralize treatment.
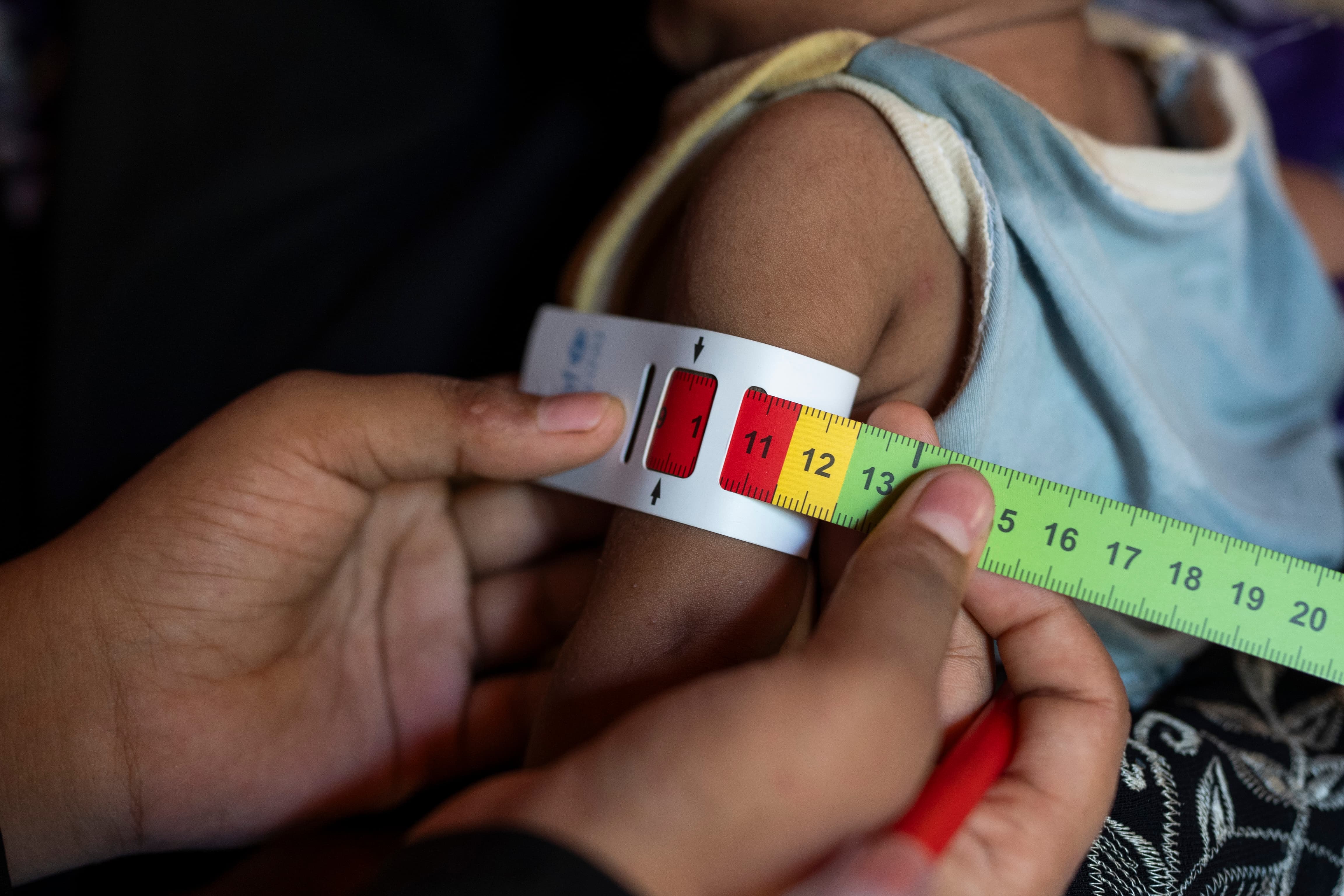
With limited access to physical treatment centers, the solution would eventually involve bringing the screening and treatment process to the patients. Traditionally, healthcare workers at treatment centers screened for malnutrition using the standard of weight against height. On a community level, this is difficult to do as the equipment is not easily affordable or portable. Instead, we found a solution in the form of a simple plastic strip. Collins pointed to research that supported the measure of mid-upper-arm circumference (MUAC) as a strong predictor of nutrition-based childhood mortality. Using a strip of plastic called MUAC Tape, healthcare workers could screen and diagnose children virtually anywhere with relative ease.
The Essential Ingredients
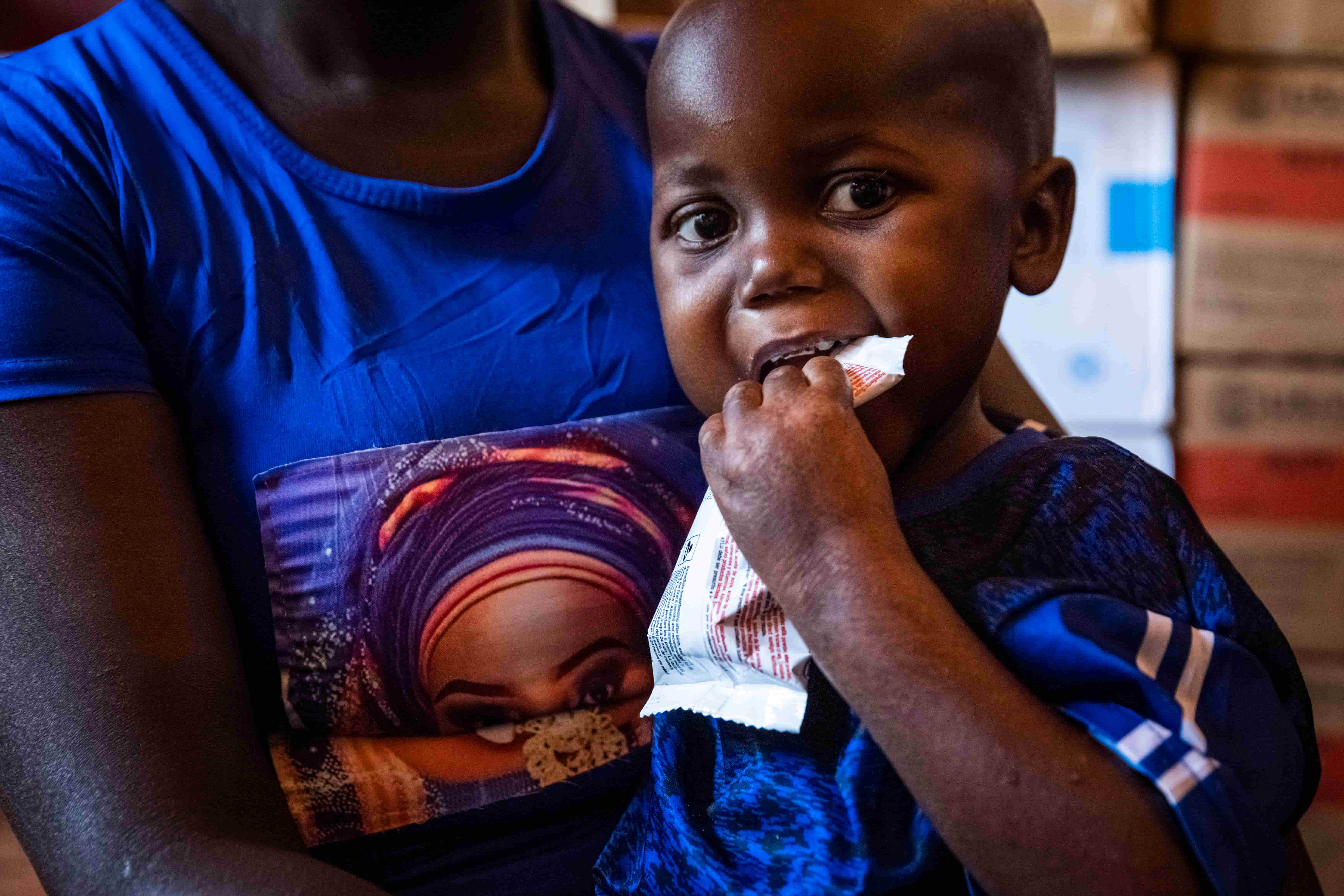
Now that we had an alternative to detecting malnutrition, our next step was treatment — which came in the form of peanuts. In 1996, French pediatrician André Briend developed Plumpy’Nut, a high-calorie, nutrient-rich, peanut-based paste. It was easier to store, had a longer shelf-life, and packed a lot of calories and nutrients in a small amount of food.
There was one last vital ingredient: Creating a treatment approach to bring these two innovations together.
“The idea was to send these children home with the correct care, so that the mothers could take care of them themselves.”
Putting It All Together
This idea became known as Community-based Therapeutic Care (CTC). With the CTC model, mothers could have their children screened close to home with a community healthcare worker and MUAC Tape. If diagnosed with acute malnutrition, they would be given the first round of therapeutic food that day and return with their child for weekly checkups. This made for a convenient yet effective method of treatment for families who struggled with the previous obstacles of malnutrition treatment.
Previous famines had resulted in child mortality rates between 10% and 30%. The pilot program of what would become CMAM saw just 4.5%.
In 2000, Concern and Valid piloted CTC during a famine in Ethiopia. While previous famines had resulted in child mortality rates between 10% to 30%, our pilot community saw just 4.5%. We tested CTC one year later in Darfur, Sudan to similar results.
Setting the Standard
CTC was initially met with resistance in the humanitarian aid community as it challenged the traditional aid model. Concern and Valid worked with Malawi’s Ministry of Health to pilot CTC at scale in Dowa district. As more mothers tested out this new model of treatment, they spread their knowledge to other mothers in the community on how to spot malnutrition and where to get help.
The program gained a valuable component: prioritizing individual agency and sharing knowledge.
By 2007, we had treated over 23,000 cases through 21 CTC programs in 4 countries. More importantly, we reached over 70% of those who needed the care, surpassing the old system’s reach of (at most) 10%.

That same year, the World Health Organization, UNICEF, and the World Food Programme issued a joint statement recognizing what we now call CMAM (Community Management of Acute Malnutrition) as a best practice, setting into motion a transformative approach that over the last two decades has saved millions of children’s lives in dozens of countries.
This revolution would not have been possible without funding from Irish Aid and USAID, operational partnerships with UNICEF and other colleagues, and — most importantly — national ministries of health, community leaders, and mothers where we worked.
CMAM Today
Over the years, we have worked with partners and communities to create more tailored approaches to community-based treatment. CMAM has continued to grow as an approach adopted by the majority of international and local agencies around the world and is used in emergencies as an approach known as CMAM Surge, a way of proactively responding to malnutrition during seasonal “surge” periods throughout the year. CMAM Surge recognizes that acute malnutrition in children often spikes during certain months of the year — whether it be during a lean period or hunger gap, or during rainy seasons that may affect food production. Having additional staff capacity and other resources on hand to respond to these spikes helps to ensure nutrition services are not overwhelmed.
Two CMAM Surge pilot tests in Kenya in 2012 saw that the model managed these peaks, without undermining other health and nutrition efforts. Since then, we’ve been rolling out CMAM Surge around the world, while also keeping an eye out for ways it can evolve in the future.
Your Support Helps CMAM Thrive
Your tax-deductible gift makes you part of a vital community that enables us to reach 9 million people each year with lifesaving nutrition solutions.
Just $50 can give a child diagnosed with acute malnutrition the life-saving therapeutic food they need.