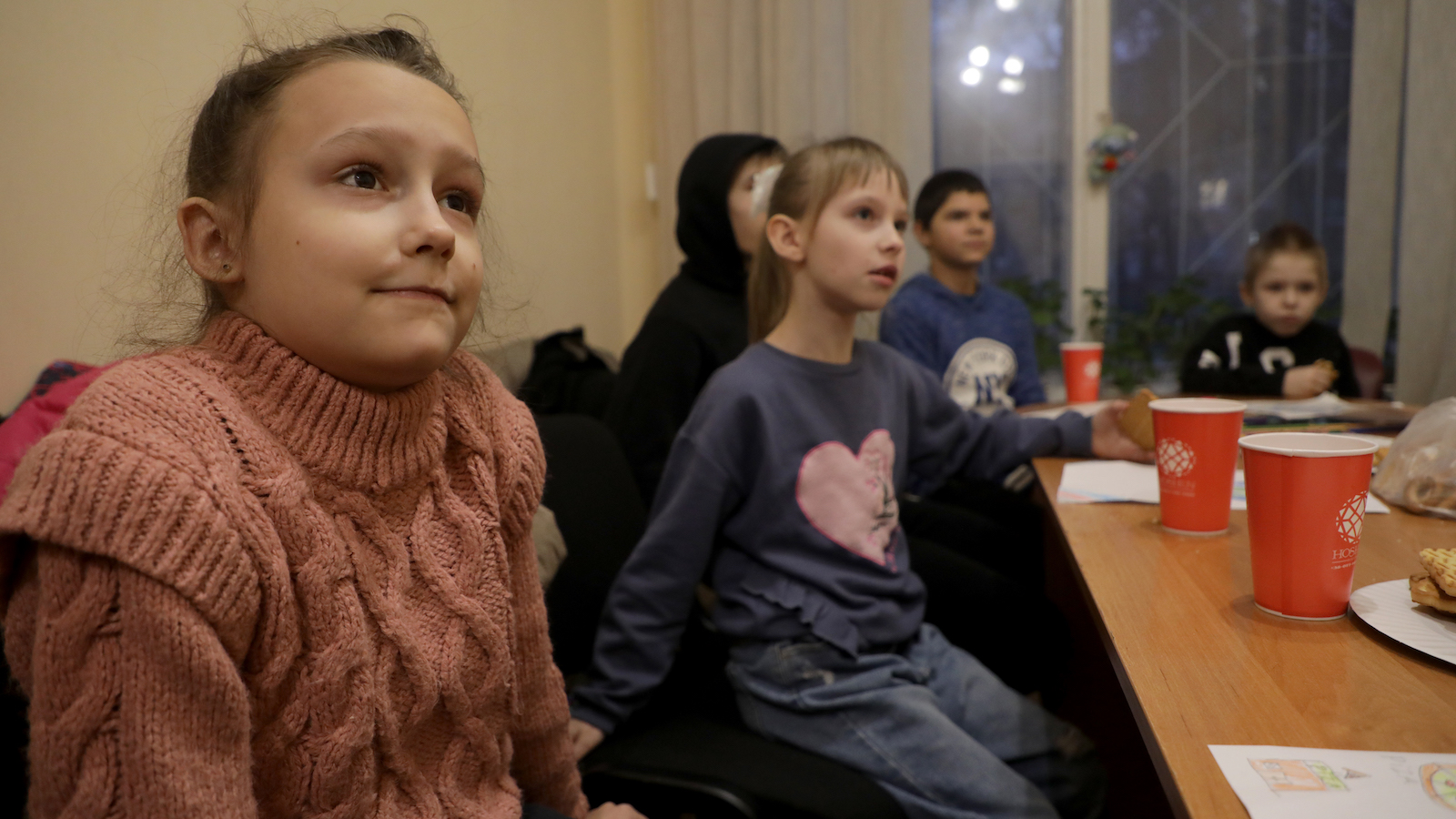Mental health and psychological support aren’t just nice-to-have in a crisis, they’re a critical factor in emergency response.
“Nobody believed this was really happening.” Veronika*, a retired tram driver, is recalling the early days of the full-scale conflict in Ukraine.
She and her husband, Olek*, watched the news play out on television and—a few days later—through their windows as tanks rolled down the streets of Polohy, a small city in the eastern oblast of Zaporizhzhia.
A steely woman of determination, Veronika’s voice nonetheless starts to break as she recalls what happened next. “At one point I looked out my window and saw a Russian soldier pointing a gun directly towards me,” she says. “He said, ‘Don’t say a word, or I’ll shoot.’ I was so scared, I couldn’t move.”
Eventually, the soldier left. But the scars remained.

When crisis hits, mental health needs surge (often just as systems break down)
Veronika’s story is sadly all too common. Each year, millions of people are caught in the middle of countless humanitarian crises and emergencies around the world, including armed conflicts and natural disasters (and, in some cases, both at the same time). The impacts of these emergencies are far-reaching: They can separate families, drive displacement, disrupt livelihoods, destroy infrastructure, and cause shortages of critical goods and services.
They also cause a huge amount of psychological distress. The World Health Organization estimates that 22% of people who have experienced war or conflict over the last decade have depression, anxiety, post-traumatic stress disorder (PTSD), bipolar disorder, or schizophrenia.

These conditions are either the result of experiencing conflict or as a pre-existing condition that has been exacerbated by the circumstances. In 2025 alone, 831 million people were directly exposed to conflict. Many of them needed support just as systems were breaking down.
Over the last 20 years, more attention has been paid to the psychological effects of a crisis and the importance of mental health in an emergency. This is true for people exposed to violence and other traumatic events, as well as people who suffer the knock-on effects of an emergency. Losing your livelihoods or home, being separated from your family, facing increased poverty levels or debt, and being unable to get adequate support are all key drivers of stress, anxiety, and depression.
An inflection point for frontline psychological support
Many countries facing the highest levels of crisis also don’t have the infrastructure to support mental healthcare, and historically it’s not been viewed as a priority in emergency response. The landscape began to change in the early 2000s, with a rise in conflict in countries like Afghanistan and Sudan. The 2004 Indian Ocean tsunami was also a major inflection point for conversations around emotional and psychological support for survivors.
In 2007, the WHO published the Inter-Agency Standing Committee (IASC) Guidelines on Mental Health and Psychosocial Support in Emergency Settings. These IASC Guidelines codified the protection and promotion of mental health and psychosocial well-being as a responsibility of all humanitarian agencies and aid workers.
The IASC Guidelines also gave us a term that is used a lot now when we talk about emergency response: psychosocial support (also abbreviated as PSS). Mental health and psychosocial support are a broad range of initiatives that organizations like Concern provide part of our duty to the emotional and psychological well-being of civilians living through crisis.
The approaches may look different based on country or context, but they’re all designed to promote well-being, alleviate distress, foster emotional resilience, and build social connectedness.

The benefits of focusing on mental health in a crisis
As the WHO writes, “mental health is crucial to the social and economic recovery of individuals, communities and countries after emergencies.”
The advantages of focusing on psychosocial support during a crisis go far beyond helping individuals (which is already a critical benefit). Here are five key benefits:
1. Psychosocial support directly aids recovery
It also reduces long-term dependency on humanitarian aid, allowing people to get back on their feet more quickly and sustainably. People who receive timely and appropriate PSS during and after an emergency are better equipped to care for themselves and their families and make decisions under stress, even in protracted situations.
2. Mental health and PSS are a force multiplier
In a crisis, psychological distress affects even the most basic aspects of daily life and humanitarian response. This includes food, healthcare, education, and shelter. Integrating PSS into these services improves the efficacy and return of broader humanitarian spending.
3. It’s also cost-effective and easy to scale
The WHO has approved of PSS being delivered by trained non-specialists, including community health volunteers. This makes it possible to provide care even in fragile contexts. Care can also be delivered through group sessions, which builds community resilience and mutual support.
4. Early response is even more effective
Timely, appropriate psychological and psychosocial response can help prevent distress and trauma from becoming more severe, meaning that the overall burden of a crisis is reduced.
This is especially true for focusing on early-age PSS for communities living through crises. Children need a different approach to counseling than adults, but providing this support can help them to live full, creative lives without the threat of lifetime or intergenerational impacts.
5. PSS supports broader development, peace, and better systems
Investing in mental health doesn’t just respond to a crisis in the moment. It can lead to permanent system gains (as was the case in Indonesia after the 2004 tsunami). PSS also supports development, human rights, and social stability at local and even national levels, aligning with broader humanitarian and development goals.

Building back better—together
About 200 miles north of Zaporizhzhia is the city of Kharkiv. Victoria* lives in a nearby suburb with her daughter Yana*. Yana is now eight, and was in kindergarten (where Victoria worked as a chef) when the full-scale invasion started.
The school sent home all students and staff, and Yana has yet to go back to the classroom. Kharkiv has become one of the frontline regions in the conflict, with constant air raid sirens and attacks. Yana has kept up with her studies online, but Victoria worries about her socialization—a key part of childhood development.
“She studies well, helps out at home, and is my friend,” Victoria says. “But she’s pretty shy and is often slow to trust people.”

Victoria signed Yana up for a child-friendly PSS group run by Concern and our partners in Ukraine. Through games, exercises, and art therapy, Yana and hundreds of other children like herself are able to connect with other kids their age and enjoy the chance to forget about everything else for a little bit.
“This program is like fresh water for the people who participate,” says Olga, a psychologist with more than a decade of experience working with children and adults. “Nowadays, communication between people is pretty limited. Sessions like these allow people to share their experiences and get some rest from the hardships of daily life.”
What does psychosocial support look like?
At its most basic, psychosocial support can look like psychological first aid in a crisis. PSS outreach creates safe, supportive environments for people affected by a crisis, helping them to rebuild routines, feel connected, and stay informed during times of uncertainty.
Psychosocial support can look like traditional one-to-one therapy and counseling sessions between a qualified provider and a patient. It can also be a group therapy session, like the ones that Yana attended, which are tailored to children. Veronica and Olek also attended PSS sessions, supported by Concern and our Joint Emergency Response in Ukraine, when they relocated to the city of Zaporizhzhia.

However, PSS is also worked into other programs, particularly education, protection, and other forms of healthcare. Many of Concern’s education programs take place in emergency contexts, and include training for teachers and caregivers to spot signs of trauma or mental distress as well as sessions to help guide children through their emotions and towards resilience. This includes spaces for what’s known as Non-Formal Education, which help children who have been out of the classroom due to crisis prepare to reenter a formal school system and have all of the emotional and mental tools to succeed.
Community mobilization and advocacy is also helpful when a crisis hits whole communities—or creates new ones amid mass displacement. In these cases, many of the impacts people face are shared, and working in group settings helps not only individual recovery, but also strengthens communities through understanding their shared challenges and struggles.

A better life
The Democratic Republic of the Congo has faced decades of crisis, including both civil war and regional violence. It was in recent years of renewed fighting that Matulizo*’s husband abandoned her and their children to fight in a local armed group.
Like many women in the conflict-struck Masisi territory, Matulizo was vulnerable in a patriarchal culture without the protective presence of her husband, unable to feed her children or afford other basic necessities. “I survived by working for others,” she says. “That’s why I decided to go to Kihanga to work the fields in exchange for a small payment.”
It was on her way home that she was confronted and assaulted by armed men. She credits Concern, however, with giving her the tools to know what to do next. Within the first few days, she went to a health center supported by Concern through the EAST Program (Enabling Affected Communities to Survive and Thrive). She knew about its services and when to go from awareness sessions that Concern teams led in her village.

As part of the EAST Program, Concern offers survivors of violence against women and girls to strengthen their resilience through livelihood training. Matulizo enrolled in this program after going to the health center, and began receiving vocational training that will enable her to start her own business, as well as ongoing psychological support.
“After my assault, I had lost the will to live. I was angry and desperate,” Matulizo says. But the program gave her hope. Once she completes her training, she’ll receive a cash transfer to support her new business. “This thought continues to lift my spirits,” she adds. “I hope for a better life.”
Help us support mental health in emergencies
Concern’s psychosocial support and mental health in emergencies work aligns with WHO recommendations and delivers care as part of our larger integrated emergency response work.
We work with local partners, trained clinicians, and skilled volunteers to deliver timely, appropriate response and ongoing support in protracted crises—in both group and individual settings. Your support can us to provide psychosocial care to people affected by conflict, disaster, and displacement by:
- Preventing or reducing psychological and social distress
- Giving children and caregivers tools to process trauma and protect themselves
- Restoring routines and learning opportunities
- Promoting physical activity and healthy daily habits
- Creating safe spaces where participants feel welcomed and supported
From play-based sessions for children to mobile support for displaced families, your tax-deductible gift enables care that addresses both visible and invisible wounds.