News
The 10 Worst Countries to Be a Mother
These are the ten countries with the highest maternal mortality rates.
Read MoreOn a world average, every woman in the 1960s had approximately five children. Today, the global fertility rate has dropped by more than half. According to the World Bank, over the last several years, women have had, on average, 2.4 children. In some countries, this decrease is even more dramatic. In Kenya, for example, the average woman in 1960 had nearly 7 children in her lifetime. In 2020, the average is now just over 3.
Currently, the United Nations Population Fund estimates that nearly 50% of all pregnancies every year — 121 million in total — are unintended. Of this figure, UNFPA executive director Dr. Natalia Kanem said that “the staggering number of unintended pregnancies represents a global failure to uphold women and girls’ basic human rights.”
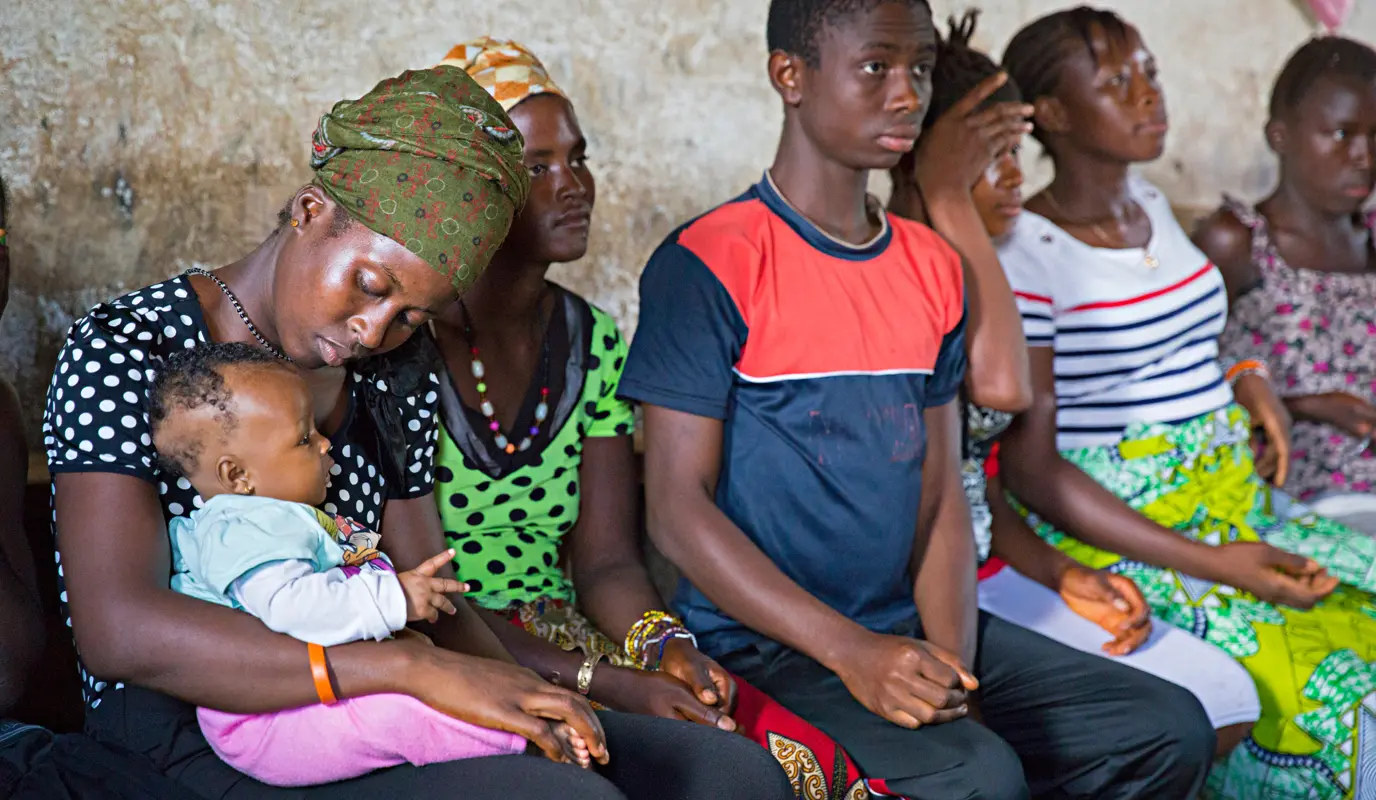
This isn’t to say that all unintended pregnancies are the result of gender inequality. However, the UNFPA reports that this is a major driver of many unintended pregnancies, especially for women who are unable to get safe and reliable contraception.
Approximately 6.5% of the world’s women want to avoid pregnancy, but are unable to do so due to a lack of access, social stigma, and harmful gender norms (among other reasons). Among them, 172 million women are using no birth control method at all. Where data is available, the UNFPA also reports nearly 25% of all women feel unable to say no to sex with their partner. “These [circumstances] all reflect the pressure that societies place on women and girls to become mothers,” concludes the UNFPA.
A crisis situation can also drive up pregnancy rates, as Dr. Kanem explains: “If you had 15 minutes to leave your house, what would you take? Would you grab your passport? Food? Would you remember your contraception?” Most people would not, and yet women are incredibly vulnerable during emergencies, especially for gender-based violence and sexual assault. The UNFPA also estimates that more than 500 women and girls in emergency situations die every day due to complications from pregnancy and childbirth.
Mónica Ferro, director of UNFPA’s Geneva office, specifically pointed to both of these figures with regards to the humanitarian crisis in Ukraine. As we have seen from the destruction of sites such as a maternity ward in Mariupol, she was unfortunately right.
“If you had 15 minutes to leave your house, what would you take? Would you grab your passport? Food? Would you remember your contraception?” — Dr. Natalia Kanem, Executive Director, UNFPA
One of the five most common causes of maternal deaths are unsafe abortions. The UNFPA estimates that 60% of unintended pregnancies end in abortion, and nearly half of these are unsafe. This rate is even higher when you look at the rates of abortion for adolescent girls (15-19). For this demographic, the World Health Organization estimates nearly 70% of all abortions are unsafe, contributing to mortality rates and, in less dire situations, lasting health problems.
While an estimated 5.9 million pregnant girls age 15-19 terminate their pregnancies, more than double that amount still give birth. More than half of them (10 million pregnancies) occur in low-income countries every year. This is often linked to child marriage. In low-income countries, 33% of girls marry before the age of 18; 12% do so before they turn 15. Many choose to become mothers due to limited options, and because motherhood is valued as a position in society, according to the WHO. However, many adolescents simply do not have the knowledge or resources for obtaining and using birth control, yet still facing the pressure to have sex, whether explicit or implicit. In some countries, the WHO reports that one-third of all women report that their first sexual encounter was forced.
While 15-19 is young, more than three-quarters of a million girls under the age of 15 (and as young as 10) still become mothers. This comes with even higher risks of complications and death as a result of pregnancy than their older peers, as girls in this age range have yet to fully develop and grow.
Despite the high maternal mortality rates that persist in many countries around the world — including the United States, where death rates are nearly twice as high as other high-income nations — 2019 was recorded as the safest year in history to give birth. Programs that improved healthcare access — from birth control to postnatal care — and legislation that protected women (especially the most vulnerable) helped to bring maternal mortality rates to a new low.
However, complications from the COVID-19 pandemic quickly undid years of progress across many sectors, including maternal health. A report by Lancet Global Health examined data from 17 countries and concluded that rates for maternal mortality, pregnancy and birth complications, and stillborn rates increased during the first year of the pandemic compared to previous years. In some cases, stillbirths increased by 28%, while maternal mortality rates increased by more than 33% in both Mexico and India. Many of these increases are seen in low- and middle-income countries, and much of it came down to women not seeking help during pregnancy out of fear of getting infected or breakdowns in overburdened healthcare systems.
Pre-pandemic, an estimated 810 women died every day due to preventable causes related to their pregnancy or childbirth. Complete data have yet to indicate whether this number has gone up due to the pandemic.
Most of these deaths can be attributed to one of five causes:
Almost all of these deaths occur in low-to-lower-middle–income countries. Part of this is due to a lack of infrastructure in many countries when it comes to healthcare, especially in remote and rural regions. Beyond this, however, pregnant and lactating mothers face a multitude of barriers when seeking care. Many cannot afford to access healthcare, receive poor quality service, or lack the information necessary to have a health pregnancy and childbirth. In some cases, harmful gender norms — such as women not being allowed to leave the house without a man’s permission or accompaniment — keep pregnant women at home and without the care they need and deserve. This is especially true for girls under 18.

There is a strong intergenerational aspect to hunger and malnutrition that begins before pregnancy. Roughly 20% of stunting in children is now attributed to malnutrition in the womb, the result of maternal undernutrition. This means even children who manage to survive being born to malnourished mothers are still less likely to reach their physical and cognitive potential in life. Breaking this vicious cycle requires, at a minimum, targeting interventions for the first 1,000 days between pregnancy and a child’s second birthday. More ideally, nutrition interventions should reach women and adolescents before they get pregnant.
Many of these issues faced by women during pregnancy and after childbirth are preventable. Between 2000 and 2017, the global maternal mortality rate dropped by 38%, from 342 deaths to 211 deaths per 100,000 live births according to the United Nations. In Southeast Asia, maternal mortality rates dropped by 59%, while countries in sub-Saharan Africa reduced their MMRs by an average of 39%.
However, the Sustainable Development Goal is to reach 70 deaths per 100,000 live births by 2030. We have more work to do.
One of the most effective ways to achieve the goal of 70 deaths (or fewer) per 100,000 live births is to simply meet the needs for reproductive health, from adolescent development through to maternal health and newborn care. A study from the Guttmacher Institute estimates this could reduce maternal mortality rates by nearly three-quarters in low-income countries.

One of the most efficient ways to meet this goal would be through midwives, many of whom can work as community healthcare professionals or as part of mobile clinics and meet 90% of the needs for pregnant women, sexually active adolescents, and newborn babies.
“When mothers understand the risks and benefits and are well supported by their community, they are more likely to seek care. It’s up to us to give them the knowledge and mechanisms they need to make healthier decisions for themselves and their families.” — Megan Christensen, Health Advisor, Concern Worldwide
Pregnancy shouldn’t be a death sentence. Based on decades of experience, Concern has adopted an integrated approach to maternal and child health. We believe that many factors influence the health of mothers and children, such as nutrition, hygiene and sanitation, environment, gender equality and attitudes, access to healthcare, and culture. Much of our work involves designing solutions with mothers (and their partners) to the challenges faced every day in the world's poorest countries. At the community level, implement those solutions daily. At the national and international levels, we take every opportunity to advocate on behalf of women and children for better health outcomes.
In Malawi, our innovative “Health Center by Phone” project (funded as part of Innovations for Maternal, Newborn, and Child Health) was integrated into the national health system, providing free access to health advice and telemedicine services in hundreds of remote communities.
In Bangladesh, Burundi, Niger, Kenya, Rwanda, Haiti, and Sierra Leone, our Child Survival programs (funded by USAID) impacted millions of mothers and young children over the past 20 years. Our research in these programs contributed to life-saving advancements in community health.
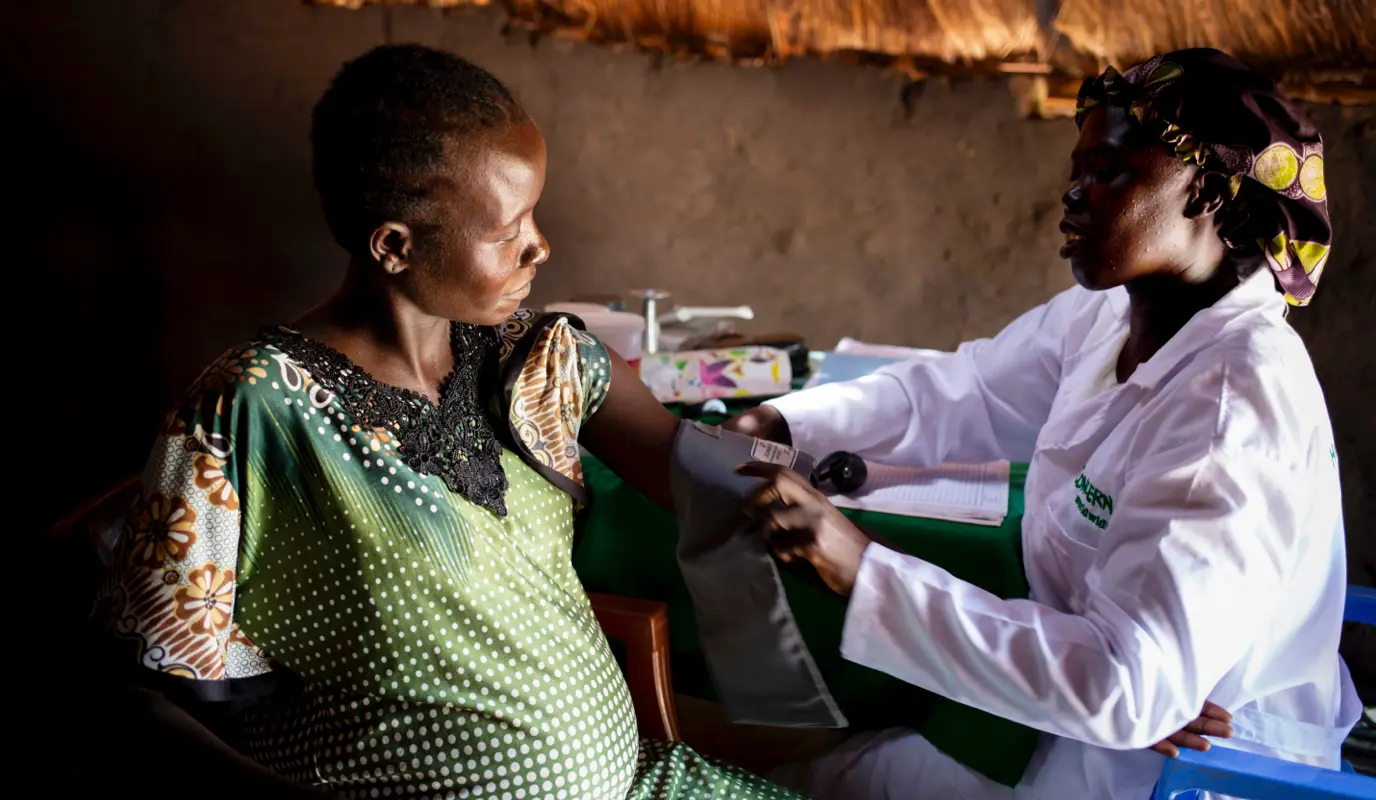
In South Sudan we have established a network of mobile health clinics providing health services to pregnant women, lactating mothers, and children under the age of 5, who otherwise would go without vital checkups or treatment, directly in their own villages.
“When mothers understand the risks and benefits and are well supported by their community, they are more likely to seek care,” explains Concern Health Advisor Megan Christensen. “It’s up to us to give them the knowledge and mechanisms they need to make healthier decisions for themselves and their families.”